BREAST DISEASES
- Diagnosis and treatment of breast masses
- Breast-conserving surgery
- Oncoplastic breast surgery (Breast reduction and breast prosthesis)
- Subcutaneous mastectomy
- Skin-sparing mastectomy
- Arm-sparing surgery and sentinel lymph node sampling
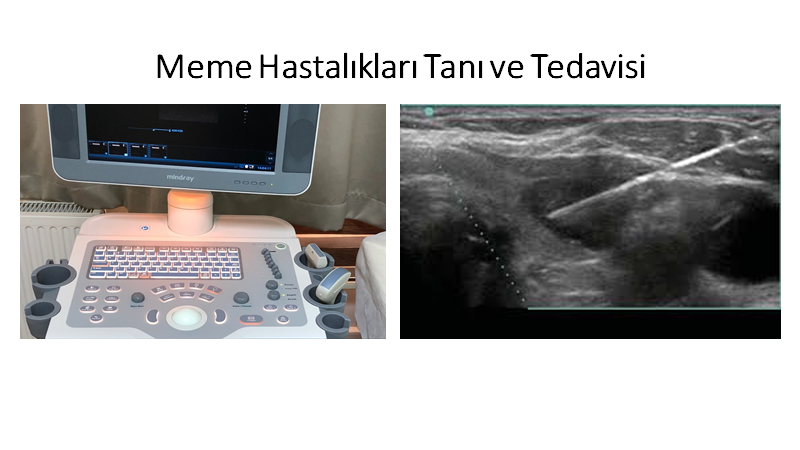
- Ultrasound-guided thick needle biopsy
- Breast ultrasound
- Follow-up and control of breast lesions
- Risk identification and consultancy
In the diagnosis of breast masses, a breast surgeon’s examination, radiological examinations (ultrasound, mammography and sometimes MRI) and breast biopsy are required. In this triple evaluation, we carry out your diagnosis and treatment in cooperation with experienced physicians. We share your treatment options with you and direct you to appropriate treatments so that you do not lose your breast. We are here to help you solve benign but difficult-to-treat diseases such as granulomatous mastitis. In the diagnosis of masses, we perform ultrasound-guided thick needle biopsy. We perform breast-conserving surgery, arm-conserving surgery with sentinel lymph node sampling, and oncoplastic surgery methods. While removing the mass, we ensure that the aesthetic appearance of the breast is preserved or pre-existing problems are corrected. We perform breast reduction and implant (silicone prosthesis) placement procedures. We also inform our patients who need to determine their breast cancer risk and receive genetic counseling. We do your annual follow-ups.
BREAST SAVING SURGERY
Breast Conserving Surgery is the removal of breast cancer with macroscopic and microscopic negative surgical margins and is called “lumpectomy,” “wide local excision,” “partial mastectomy,” “segmental resection,” or “quadranectomy.”
Breast-conserving therapy follows breast-conserving surgery with moderate doses of radiotherapy to eliminate microscopic residual disease. It is an alternative to mastectomy in patients with early stage breast cancer. Before breast-conserving therapy, all breast cancers were treated with mastectomy. Although contemporary surgical techniques cause less morbidity than radical mastectomy, mastectomy causes breast loss. The goals of breast-conserving therapy are to provide life expectancy equivalent to mastectomy, a beautiful-looking breast, and a low recurrence rate in the treated breast.
There is no difference in terms of life expectancy between breast-conserving treatment and complete breast removal. The advantage of breast-conserving treatment over mastectomy is the better cosmetic and psychological outcome.
The disadvantage is that the risk of tumor recurrence in the remaining breast tissue is slightly higher than if the entire breast is removed. If the tumor recurs in the breast that received preventive treatment, the recommended treatment is mastectomy, that is, removal of the entire breast. Local recurrence of the tumor does not have a negative effect on survival time.
LUMPECTOMY: It is the removal of the breast skin above the lesion and the removal of the lesion to wide limits (>=1 cm) down to the underlying fascial layer.
TUMORECTOMY/WIDE LOCAL EXCSION: It is simply the removal of the entire lesion. There is no need to remove skin or delve into fascia.
QUARANECTOMY: The quadrant where the tumor is located is removed along with the skin and underlying fascia with a 2-3 cm surgical margin. The risk of positive surgical margins is low, but the cosmetic results are poor.
PATIENT SELECTION — Although breast-conserving therapy is a good alternative to mastectomy, it cannot be performed in all patients. Selection of appropriate patients is important in the success of breast conserving therapy. Most contraindications are due to inability to achieve border control with breast-conserving therapy or inability to tolerate adjuvant radiotherapy.